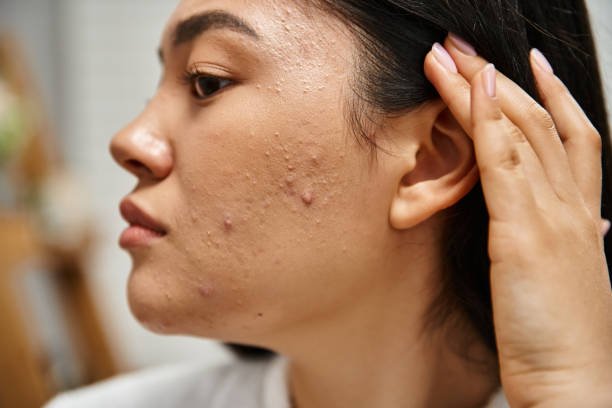
No one can deny the fact that changes in the skin during perimenopause can be uncomfortable and frustrating. The majority of women nowadays are living approximately 30 years into post-menopause, so the issue of maintaining healthy skin is of long-term concern.
Perimenopause acne is one of the most common problems that many women experience at this age. In contrast to teenage acne, this kind of acne appears later in your life and frequently on the lower face, jawline, and chin.
It is worth mentioning that not all women get acne in perimenopause. But if you are dealing with breakouts and cannot point to any obvious cause, perimenopause may be the culprit.
What Is Perimenopause Acne and How Does It Differ from Other Acne
Perimenopause acne is a form of breakouts that develops during your perimenopause stage, which is simply a transition phase before menopause.
This period may begin in your 40s, or even late 30s, and continues up to menopause. During this period, your hormone levels, especially estrogen and progesterone, fluctuate greatly. These changes may enhance androgen activity and activate the sebaceous (oil) glands in your skin. This oil overload may block your pores and cause acne.
- Location: These types of acne are usually located in the lower part of your face, jawline, chin, and neck, and not on the forehead or the T-zone.
- Pattern: It is often cyclical and may flare during times of stress, hormonal shifts, or certain foods.
- Appearance: It appears as deep, inflamed, or cystic lesions and is more prevalent than either blackheads or whiteheads.
- Persistence: These types of acne occur even if you had clear skin in your younger years.
Acne is mostly brought about by bad hygiene or cosmetic products, but perimenopause acne is caused by your hormonal fluctuations. That is why topical treatments cannot be quite efficient for perimenopause acne.
Key Causes of Perimenopause Acne
1. Hormonal Fluctuations
As already mentioned, your fluctuating hormones during perimenopause are the most significant and primary source of perimenopausal acne. In fact, the whole topic of adult and perimenopausal acne is now regarded as a chronic inflammatory process caused by hormonal fluctuations rather than the oil production caused by the traditional teenage acne process.
2. Weak Skin Barrier in Your 30s & 40s
The most important hormone that helps to keep your skin thick, elastic, hydrated, and with a solid barrier is estrogen. When your estrogen levels drop with perimenopause, your skin barrier weakens and becomes drier. And that isn’t typical of acne in youth
A compromised barrier means tiny cracks and weakened defenses that let bacteria and irritants penetrate your skin more easily. This will cause inflammation and even acne in areas where it is not typical.
If this is your cause, you must include more barrier-repair skincare, such as hydrating moisturizers or ceramides, and do not use products that strip off all the oil, such as harsh scrubs or alcohol-based acne washes.
3. Less Good Bacteria on Your Skin
As you age and perimenopause progresses, your skin bacteria levels change. Scientific studies confirm that the proportion of good and bad bacteria present on your skin surface is out of balance. This means that the levels of good bacteria may be reduced, and those bacteria associated with acne may take over your skin surface.
As a result, your skin may become more inflamed, and pores may clog, thus resulting in acne.
In this case, a prebiotic or probiotic cream and cleanser may be good for you.
4. Redness and Rosacea-like Reactions
Some women in their 45s may see redness and inflammation, known as acne rosacea. It is a separate, chronic condition involving inflammation of dilated blood vessels.
If you experience redness and breakouts, anti-rosacea medications may be more effective than your regular anti-acne medications. This includes anti-rosacea medications such as azelaic acid, metronidazole, or ivermectin.
5. Skincare and Medications
If you are using harsh skincare products, heavy creams, or certain medications like steroids or hormone therapy, these can also irritate your skin.
Real Remedies for Perimenopause Acne
Since perimenopause acne is not so severe, there are some home remedies and steps you can take to manage it nicely:
Wash your face twice a day: It is always best to wash your face twice a day with a non-foaming face wash. Try to avoid using face wash or scrub that contains chemicals, as they can cause your face to lose its natural oils. It is always best to wash your face with lukewarm water, not hot water. If you have an acne-prone face, you can go for a face wash that contains salicylic acid.
Moisturize: Don; forget to moisturize after cleansing and use a non-comedogenic face moisturizer that contains ceramide or hyaluronic acid.
At-Home Spot Treatments: Use Aloe vera gel to soothe your face. You can go for Green tea extract or Honey or a manuka honey face mask. Use ice packs to soothe your face if you have a cystic acne problem
No Popping: Avoid picking or squeezing pimples. This can worsen your inflammation and increase redness, especially if rosacea-like reactions are present.
Eat more gut-healthy meals: You can include probiotic-rich foods like yogurt, kefir, or fermented vegetables. Also, some prebiotic fibers from foods like bananas, onions, and garlic feed good bacteria and may reduce inflammation.
Simplify Your Skincare
You only need a handful of active ingredients. Don’t waste your money on a 10-step acne routine. It will only irritate your skin more. You can choose one or two of the following:
Salicylic Acid (BHA): This is your best friend. It dissolves oil and gets deep into your pores, cleaning out clogs. Use a cleanser with salicylic acid every night, or use a toner pad with salicylic acid a few times a week.
Benzoyl Peroxide: This kills the bacteria that cause your pimple to become red and inflamed. Use a 2.5% or 5% benzoyl peroxide treatment directly on your pimple at night.
Retinol: This accelerates cell turnover, keeping dead skin cells from clogging pores. It’s also the best anti-aging product out there. Use a pea-sized amount all over your face 2-3 nights a week. If you use retinol, you must use sunscreen in the morning.
Medical Treatments (When to See a Doctor)
In case you have used drugstore medicine for 2-3 months and your acne remains painful or leaves scars, it is time to make a call to a dermatologist or your gynecologist. The following medical interventions actually work on perimenopause acne:
- Prescription Topicals: Your doctor will give you stronger doses of what’s in the store. These can be tretinoin (retin-A) or topical antibiotic gels that contain Clindamycin. These kill bacteria on your skin without the side effects of antibiotic pills.
- Oral Medications: Your doctor may give you some anti-androgen or antibiotic pills that will reduce oil production.
- Hormone Replacement Therapy (HRT): As low estrogen is the cause of the perimenopause acne, hormone replacement therapy is used to restore the level of estrogen. Your doctor will give you an estrogen patch, pill, or gel.
- In-Office Treatments: If your acne has left scars, then a dermatologist can also recommend a hydrafacial or chemical peels. If you have a big, painful cystic pimple that needs to be gone tomorrow, then your doctor will give you cortisone injections, a tiny amount of steroid, and it will be gone in 24 hours.
Conclusion.
Perimenopause acne is a temporary condition, and once your hormones calm down, your acne will clear up. Until then, you need to take care of your skin and be patient with your treatments.
You can easily do this by learning what causes your acne and following a routine that helps prevent and heal your acne, and keep your skin healthy during your perimenopause period.
At Kairos Health and Wellness, one of our functional nurse practitioners, Lola, helps women in Houston and throughout Texas overcome perimenopause acne with a holistic approach.
Book your appointment today!